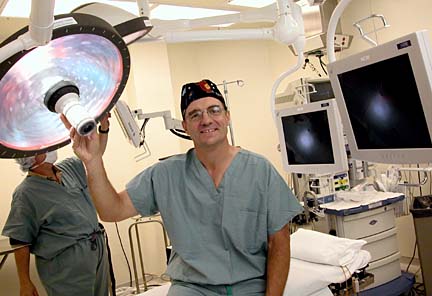
Dr. Daniel Robie, medical director of Kapiolani Medical Center's advanced minimally invasive services, stands in an operating room equipped with the latest technology.
Doctors relish
own reality TVVisiting specialists on Maui watch
a live feed of video camera-probe
surgery at Kapiolani
Six children underwent surgery in Honolulu that was watched by about 250 surgeons gathered in a Maui hotel.
The operations were done at Kapiolani Medical Center for Women and Children last week during a telesurgery workshop at the Wailea Marriott Hotel.
"In the exact words of some physicians, everything went 'just perfectly,'" said Maggie Cabastas, manager for Kapiolani perioperative services. "The kids are all fine."
The workshop highlighted the 13th annual Congress for Endosurgery in Children held on Maui by the International Pediatric Endosurgery Group to focus on the latest advances in the field. Surgeons attended from 23 countries.
It was the first time in the organization's history that live surgery was performed during the meeting so participants could watch and ask questions.
The operations were performed simultaneously last Thursday in two state-of-the-art surgical suites dedicated to minimally invasive procedures at Kapiolani. One is new, and the other has been refitted with the latest technology and computerization.
Rather than traditional open surgery, minimally invasive techniques involve small incisions and small surgical instruments with laparoscopic or endoscopic instruments to see inside the body.
Patients in the telesurgery workshop were infants and school-age children from Honolulu, Maui and the Big Island with different congenital defects involving the stomach, lower intestine, hernia and lungs. The most complex case took about three hours.
Dr. Daniel Robie, Kapiolani's medical director of advanced minimally invasive services, and five internationally recognized guest surgeons performed the procedures.
They were Drs. Keith Georgeson, Alabama Children's Hospital; Craig Albanese, Stanford University; Thom Lobe, Memphis Children's Hospital; Steve Rothenberg, Presbyterian St. Luke's Hospital; and C.K. Yeung, of Hong Kong, president of the Endosurgery Group.
Robie began minimally invasive pediatric surgery at Kapiolani in 1999 and has operated on patients as young as 24 hours.
"We really kicked into full speed, taking more advanced procedures, in 2000," he said.
With the recent changes, he said, Kapiolani's surgical suites, used for adult and pediatric cases, have capabilities others lack for the most advanced minimally invasive procedures. "We are now on a par with the best centers on the mainland."
Robie said the rooms have an "integrated operative environment" giving the surgeon control over the monitors he or she must look at while doing surgery to see inside the body, as well as most other facets of the surgery.
By pressing touch screens, for example, the surgeon can change the room's lighting, the patient's abdominal pressure, the size of the operating area or the table position.
The surgeon also can change settings, make telephone calls, turn on the video or DVD and get still images to record the operation for educational purposes or to share with families.
"I can actually scroll through different pages that control different pieces of equipment," Robie said, demonstrating the sophisticated technology.
Previously, he said, nurses had to scurry around the room changing monitors and pressing buttons to change settings on the machinery.
"Most of the time now, nurses are able to sit in the corner and oversee goings-on in the room. It saves on personnel," he said.
The surgeon also can custom-design the room for a particular operation, moving the monitors anywhere needed for the operating area, he said.
The previous methods were not nearly as ergonomically effective, Robie said, "plus, it wasn't in my control at all. This is much better; and we had no telemedicine capabilities. It is all new."
The telemedicine system, added April 5, enables surgeons at Kapiolani to consult with experts around the world who can observe operations and provide feedback, Robie said.
This will reduce the need to send complicated cases to the mainland and avoid travel expenses and long separations for families of patients, he said. "We will still need an occasional transfer, but it extends our capabilities."
Dale Moyen, the telemedicine program manager who set up the telesurgery workshop, said, "Everything went off without a hitch." Surgeons in the audience on Maui asked questions, and those doing the operations at Kapiolani Medical Center responded, he said. "It was really neat."
Moyen said telemedicine "is a great tool for continuing education" for medical residents. They previously had to observe surgery in the operating room, he said. "Now they can be at UH or the auditorium or anywhere and observe for credit."
Suzann Filleul, Kapiolani director of perioperative services, said minimally invasive procedures have been used a long time for adults, but the technology has been a little slower for children because they are so small.
She said "it's wonderful" for the surgeons and staff and for the patients because it is less painful, with a faster recovery.
"We love it. It's so nice to be able to do things like this for our children."
BACK TO TOP |
Brigitte Grainger, 8, right, and her brother, Jimmy, 6, have a genetic disorder affecting the blood cells that required the removal of their spleens to avoid blood transfusions every month. With them are sister Rachelle, 16, left, and mom Sandra.
Family learns benefits
of new surgery
Sandra and James Grainger, of Honolulu, can vouch for the benefits of minimally invasive surgery.
Two of their three children -- Brigitte, 8, and James, 6 -- have spherocytosis, a hereditary disorder of the red blood cells.
Without surgery, they would need blood transfusions every four to six weeks, Sandra Grainger said.
She said Brigitte "kept getting paler, like yellowish tint," at about 8 months old. A blood specialist at Kapiolani Medical Center for Women and Children diagnosed her condition.
Her spleen was removed at Kapiolani when she was about 3 years old in a traditional surgical procedure with a regular incision, her mother said.
"She was five days in the hospital, and when she got home, it took a while to recover. Even after a year later, she complained that her scar would hurt."
She said a geneticist told the couple there was a 25 percent chance another child would have the same disorder, although Rachelle, 16, does not have it.
Jimmy was diagnosed with the condition at birth and required a blood transfusion the first week after he was born, Grainger said. However, he did not require as many transfusions as Brigitte, she said. "For some reason, his blood cells were lasting longer."
Minimally invasive surgery was being done at Kapiolani when his spleen was removed in March last year.
"It was a major difference," his mother said. "He only stayed in the hospital two days, and maybe a couple days after he was home, he was up and trying to run around. You wouldn't think he went through any surgery at all, and there's no incision, just three little points.
"My daughter's got a pretty big scar on her stomach," she said, compared with "just three little dots. They look like mosquito bites. There is quite a big difference between the two surgeries."
Both children are "doing very well," she said. Brigitte is in third grade and Jimmy in kindergarten at Makalapa Elementary School.