Researching doctors
can be hard taskA recent botched surgery
reveals how little patients
learn about doctors' pasts
Dr. Robert Ricketson knew the spine surgery he performed on Jennie Young for back pain had gone terribly wrong.
He faced Young's husband in the waiting room of an Oklahoma hospital and told him that he had "severed eight or nine nerves and that he could not adequately express how sorry he was," according to court documents.
COURTESY PHOTO
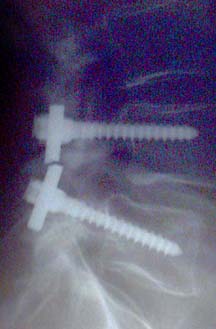
An X-ray shows the shattered pieces of a screwdriver used in a botched spinal operation on Arturo Iturralde.
"Dr. Ricketson even drew a picture of the problem for Mr. Young," said Mark Bonner, the Youngs' attorney.
After the 1997 operation, Young was partially paralyzed, forced to wear diapers and today can walk only with a walker.
In May 1998, a month after the Youngs sued Ricketson, alleging he was high on narcotics during the botched surgery, the Oklahoma surgeon applied for and was granted a new medical license in Hawaii.
With at least five malpractice suits against him and Oklahoma requiring drug testing, Ricketson began practicing on the Big Island. Hawaii Orthopaedics Inc. in Hilo hired him as a spinal surgeon, and he was granted surgical privileges at Hilo Medical Center.
Ricketson's case illustrates how little consumers know about the skills, malpractice histories and possible impairments of the physicians who hold their lives in their hands. Consumers have limited access to such information and they often don't inquire about their doctors' qualifications with state regulators.
By the time Hilo resident Arturo Iturralde was strapped onto Ricketson's operating table Jan. 29, 2001, the former Oklahoma surgeon had been sued for malpractice seven times, he'd paid the Youngs $1.3 million, Texas had revoked his license and Oklahoma had temporarily suspended it before placing him on probation, according to documents from two states.
According to a wrongful death lawsuit filed earlier this month, Ricketson was about an hour into Iturralde's back surgery when he discovered the titanium rod he intended to implant was missing.
The suit alleges that Ricketson grabbed a stainless-steel screwdriver, used a hacksaw to cut off the handle and a piece of the blade, and then inserted the piece into Iturralde's spine.
Days later, the screwdriver snapped in half.
Iturralde died June 18 at age 76, a bed-ridden paraplegic who depended heavily on pain killers and the care of his sister, Rosalinda.
Richard Peterson, a Big Island attorney for Ricketson's employer, Hawaii Orthopaedics, which was also named in the suit, said extensive checks are done on physicians who are hired.
"At one point in Dr. Ricketson's past, he had an addiction to pain killers as a result of back surgery. And as far as anybody knew here, he had had no further problems in that regard," said Peterson, "He got help years ago and he appeared to be fully recovered from any addiction."
Patients who want to investigate the histories of physicians, which could include drug or alcohol addictions, will find much information is closed to the public and only available to certain medical professionals.
Aside from surfing the Internet for news accounts of malpractice suits or checking a few Web sites (such as www.questionabledoctors.org), local consumers must rely on the judgment of the Hawaii Medical Board and the Hawaii Medical Association's Committee on Physicians' Health, a peer-review group.
The board, which can grant and revoke medical licenses, bases many of its actions on the Physicians' Health committee that monitors its own for problems ranging from drug addiction to old age.
"For the most part, patients are really in the dark about their doctors and surgeons," said Richard Miller, a former law professor at the University of Hawaii and a consultant to the Hawaii Coalition for Health, a nonprofit patient-advocate group.
"People should be able to get accurate up-to-date data about the past experience of the physicians," he said.
Miller acknowledged that there are many frivolous malpractice suits and it is an unfair way to judge the abilities of a physician.
He also said that many patients are reluctant to dig into their doctor's background. "People want to think their doctors are wonderful and can do no wrong. It's a societal thing about how we view the position of doctors and ourselves as patients."
At the national level, Congress set up the National Practitioner Data Bank in 1991 so that hospitals and other medical professionals can effectively track doctors anywhere in the country for license revocations, disciplinary actions and payouts in malpractice suits from judgments or settlements. Counting only suits with payouts is an attempt to factor out frivolous lawsuits.
By law, any physician who has been disciplined by a hospital or state medical board or made any kind of payment for a medical malpractice suit must report it to the data bank.
But the system has loopholes. For example, if a disciplinary action is less than 30 days long, it can go unreported. And military doctors do not report to the data bank.
The data bank, which tracks more than 215,000 questionable doctors and dentists, was designed to make it difficult for doctors to skip from state to state.
But the public can't get the information in the data bank. HMA President-elect Dr. Inam Rahman said the data bank should be closed to the public to protect the confidentiality of patients and doctors.
Rahman said if the data bank was public, physicians would not voluntarily report to it and there would be no effective way for hospitals and medical practices to screen physicians.
At the state level, the Regulated Industries Complaints Office is the enforcement arm for the medical board, overseeing the disciplining of professional licenseholders from doctors and contractors to Realtors and beauticians.
Jo Ann Uchida, complaints and enforcement officer for RICO, said staff can tell a consumer if a doctor's license has been revoked or suspended or if the medical board has made any formal order. Her staff is not allowed to characterize a disciplinary action, but consumers can request a copy of any written order.
Uchida said that of the 95,621 inquiries consumers made to RICO last year, most concerned contractors and only 5,200 were about physicians.
The Hawaii Medical Board depends heavily on the HMA's Physicians' Health Committee. Comprised primarily of physicians, the committee has five members who are certified by the American Society of Addiction Medicine to deal with substance abuse, alcoholism and other health problems.
"We have a highly educated, highly skilled bunch of people who are very knowledgeable about dealing with impairments," said Dr. Larry Schlesinger, committee chairman.
Schlesinger said the committee gets complaints about impaired physicians from patients, fellow doctors, hospitals, health care professionals and even family members. The committee intervenes quickly and, if necessary, puts the doctor into treatment. The physician is asked to sign a contract with the committee that sets down strict rules, usually for a five-year probation period.
If substance abuse has been the problem, the physician must continue some form of treatment, submit to weekly random drug tests and see a therapist. A physician unable to do this is reported to the licensing board and revocation is recommended.
"We have tight controls and a big stick," said Schlesinger, "We have stringent contracts, weekly drug testing and if someone is using we find out pretty fast. And if someone doesn't follow the rules we lay down for them, we have a big stick to use: They lose their license."
But again, the work of the committee is confidential.
Schlesinger defended the confidentiality: "We keep close tabs on doctors. But we need to be able to deal directly with the doctors and have them feel free to communicate with us and not be afraid that things they say will show up on the front page of the newspaper."
Schlesinger said the committee has successfully signed monitoring contracts with physicians, but if the proceedings were public he doubts many would sign. Schlesinger declined to say how many of Hawaii's 1,600 to 1,800 practicing physicians are under contract.
He said, "We have helped so many physicians to reclaim their lives, and we have helped the community not to lose good doctors because of their medical problems."
Stating he could not divulge details of the Ricketson case, Schlesinger said: "I feel the system is working and we are able to get physicians into treatment. We watch them closely for substance abuse and see to it they have a therapist and someone else they can talk to. We keep very close tabs on them for substance abuse. But this is an obvious case of just poor judgment and we have no way of controlling that portion of a physician's life."
If Iturralde, a Baptist minister who spoke mostly Spanish, had called RICO, he could have requested a copy of the settlement agreement the state signed with Ricketson on Nov. 17, 2000, about two months before his back surgery.
Iturralde would have learned from the agreement that Ricketson was being monitored by the HMA's Physicians Committee as early as March 1999, almost 20 months before the Hawaii Medical Board fined him $500 and put him on four years probation in November 2000.
But he would not have learned why he was monitored.
The agreement lists the Oklahoma suspension and the Texas revocation and says that the board took action against Ricketson because he failed voluntarily to report those disciplinary actions to the Hawaii board.
While the agreement indicates a concern about Ricketson it does not identify the problem. Iturralde would have needed to see the Oklahoma board's documents to find out about Ricketson's admitted drug addiction.
According to documents from the Oklahoma Board of Licensure and Supervision, Oklahoma opened an investigation of Ricketson on Oct. 5, 1998, which was several months after he moved to Hawaii.
During the course of the investigation, Ricketson underwent in-patient treatment twice and admitted that he was addicted to narcotics from January 1997 until June 1998 (during the time of Young's surgery). He also admitted that he wrote fake prescriptions to get drugs.
On Dec. 14, 2002, Ricketson went before the Kansas State Board of Healing Arts to get a new medical license, according to documents from that state.
After reviewing his record, the Kansas Board advised him to withdraw his application. On Dec. 18, 2002, Ricketson withdrew.
Ricketson could not be located for comment about this story.
History of a doctor's malpractice lawsuits
>> July 1, 1988: Ricketson issued Oklahoma medical license.
>> Nov. 14, 1992: Ricketson issued Texas medical license.
>> July 5, 1993: Ricketson opens solo practice in Edmond, Okla.
>> Sept. 8, 1995, to May 30, 1996: Four medical malpractice lawsuits are filed against Ricketson in Oklahoma.
>> April 16, 1998: Jennie Young files malpractice suit in Oklahoma after an operation performed by Ricketson leaves her partially paralyzed.
>> May 11, 1998: Ricketson applies for Hawaii medical license and is accepted.
>> Oct. 5, 1998: Official complaint filed with Oklahoma Board, which starts investigation.
>> Nov. 2, 1998: Ricketson admits drug addiction to Oklahoma Board. He attends inpatient treatment from Nov. 2, 1998, to Dec. 11, 1998.
>> Jan. 5, 1999: New malpractice suit filed in Oklahoma.
>> Jan. 21, 1999: Ricketson's license is suspended in Oklahoma for 60 days, and he is put on probation for five years.
>> Feb. 2, 1999: New malpractice suit filed in Oklahoma.
>> March 1999: Ricketson meets with the Hawaii Medical Association's Committee on Physicians Health and agrees to be monitored under the same terms of the Oklahoma order, which includes drug testing.
>> March 30, 2000: Texas State Board of Medical Examiners revokes Ricketson's medical license.
>> Nov. 18, 2000: Hawaii Board of Medical Examiners signs a settlement agreement with Ricketson that puts him on probation for four years and requires random drug testing and other conditions.
>> Jan. 29, 2001: Ricketson operates on Arturo Iturralde and allegedly puts a piece of a screwdriver into his spine instead of a titanium rod. A few days later, the piece of screwdriver snaps. Despite several corrective surgeries, Iturralde is left a paraplegic.
>> Late 2001 or 2002: Ricketson applies for a Kansas medical license.
>> Dec. 14, 2002: Kansas Board of Medical Examiners recommends that Ricketson withdraw his application for a medical license. He does.
>> June 18, 2003: Arturo Iturralde dies.
>> July 14, 2003: Rosalinda Iturralde, Arturo's sister, files a malpractice and wrongful death suit against Ricketson, Hawaii Orthopaedics, Hilo Medical Centers and others on the Big island.
BACK TO TOP |
Group says isle board fails to properly discipline doctors
Hawaii's medical licensing board has the worst record in the country when it comes to disciplining doctors, according to Public Citizen, a consumer advocacy group founded by Ralph Nader.
Constance Cabral, executive officer of the Hawaii Board of Medical Examiners, declined to comment on the findings.
Public Citizen recently reviewed data from the Federation of State Medical Boards to rank the 50 state boards and the District of Columbia based on the rate of disciplinary actions against doctors in 2002.
To factor out frivolous lawsuits, Public Citizen included medical malpractice suits only when a physician made a payout in either a settlement or judgment.
Hawaii ranked 51st, behind Delaware, Wisconsin, Tennessee and South Carolina. Hawaii also ranked among the lowest states in 2001 and 2000.
"Hawaii is one of the worst boards in the country," said Dr. Sidney Wolfe, director of Public Citizen's Health Research Group.
Wolfe said Hawaii had 1.07 disciplinary actions per 1,000 physicians, compared to the national average of 3.56 actions per 1,000.
Wolfe said a low discipline rate does not mean a state has more competent doctors. He said the low rate is an indication that the board is not investigating or taking action.
Wolfe was critical of Hawaii's discipline of doctors with two or more payouts (either settlements or judgments) in medical malpractice suits. Public Citizen found that between 1990 and 2002, 71 Hawaii doctors each made payouts in two or more malpractice suits. Of those, only six doctors, or 8.5 percent of the group, had actions taken against their licenses by the Hawaii Board of Medical Examiners.
Of the 19 doctors with three or more payouts in the same time period, the Hawaii board took licensing action against three, or 15.8 percent of the group.
"Boards that don't take action against questionable doctors are usually underfunded and don't have the resources -- or don't choose to have the resources -- to check the doctors out," Wolfe said. "They don't take advantage of the instantly available electronic databases that show which doctors are in trouble or getting into trouble."
BACK TO TOP |
Resources to investigate doctors
Consumers interested in checking out a physician can check these online databases. All charge fees for the service.>> www.questionabledoctors.org: This site is maintained by Public Citizen, a group founded by Ralph Nader, and had the most information on Dr. Robert Ricketson. It listed 119 doctors in Hawaii with actions against them.
>> www.choicetrust.com: This site is maintained from public documents by ChoicePoint of Alpharetta, Ga.
>> www.healthgrades.com: This site uses public documents and its own proprietary grading system from Health Grades Inc. of Lakewood, Colo.